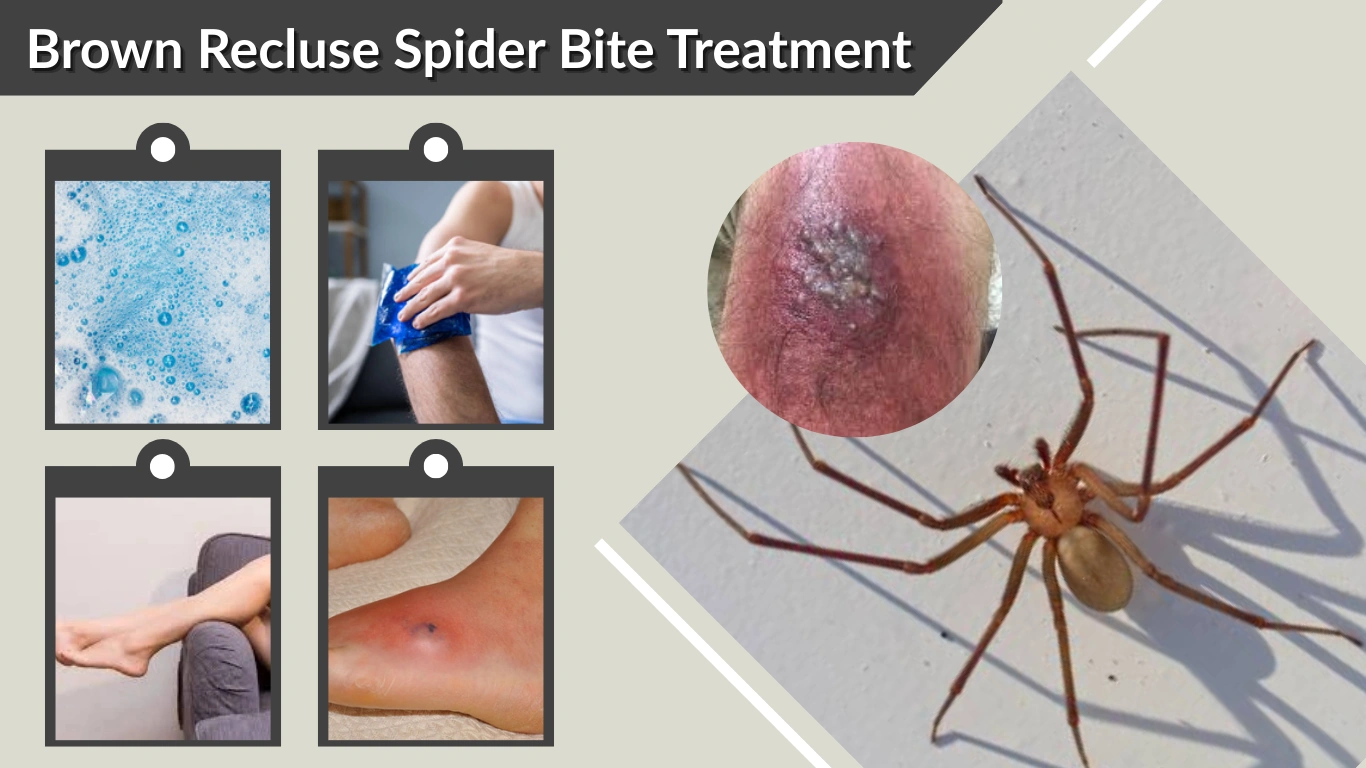
Brown recluse spider bites require a careful, measured treatment approach focused on symptom control, wound protection, and close monitoring. While many bites remain mild, others can progress over several days, making early and appropriate care essential. This first half of the article covers initial treatment, medical evaluation, and early-stage management, which together form the foundation of effective recovery.
Understanding the Treatment Approach
There is no specific antivenom for brown recluse spider bites. Treatment is primarily supportive, meaning it aims to reduce pain, limit tissue damage, prevent infection, and manage complications if they arise. Importantly, aggressive or unproven treatments can worsen outcomes, so restraint and observation are often key components of care.
Immediate First Aid After a Suspected Bite
Prompt first aid can help limit the severity of symptoms, especially within the first 24 hours.
Clean the Bite Area
- Gently wash the area with soap and clean water
- This reduces the risk of secondary bacterial infection
- Avoid scrubbing, which may irritate the skin further
Apply Cold Compresses
- Use a cold pack or ice wrapped in a cloth
- Apply for 10–15 minutes at a time, several times a day
- Cold helps reduce inflammation and may limit venom activity
- Heat should be avoided, as it can worsen tissue damage
Elevate the Affected Area
- If the bite is on an arm or leg, keep it elevated when possible
- Elevation helps reduce swelling and discomfort
Avoid Harmful Home Remedies
Do not:
- Cut the bite open
- Attempt suction
- Apply heat
- Use bleach, chemicals, or herbal pastes
These practices have no proven benefit and can increase tissue injury.
When to Seek Medical Evaluation

Medical evaluation is recommended if:
- Pain or redness worsens after 24 hours
- A blister, ulcer, or darkened skin develops
- The bite occurs in a child
- Fever, nausea, or fatigue appears
- The wound does not improve over several days
Because many skin conditions mimic spider bites, clinicians often focus on symptom patterns and progression, not just appearance.
Diagnosis and Assessment
There is no laboratory test that confirms a brown recluse bite unless the spider is captured and identified. Healthcare providers typically:
- Review symptom timeline
- Examine the wound’s appearance
- Rule out bacterial infections, allergic reactions, and other insect bites
Accurate diagnosis helps avoid unnecessary antibiotics or procedures.
Early Medical Treatment (First 24–72 Hours)
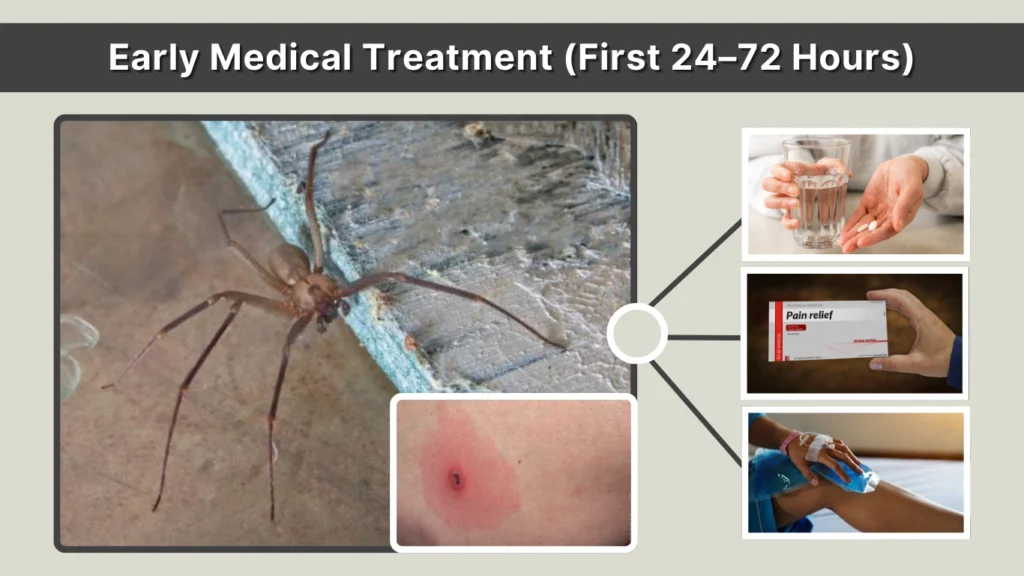
Pain Management
- Mild pain: acetaminophen or ibuprofen
- Moderate to severe pain: prescription pain relief may be required
- Aspirin is usually avoided in children
Anti-Inflammatory Care
- Cold therapy remains the primary anti-inflammatory measure
- Steroids are not routinely recommended and are reserved for specific cases under medical supervision
Tetanus Protection
- A tetanus booster may be given if immunizations are not up to date
Monitoring Progression
- Patients are often advised to mark the edges of redness
- Daily checks help track expansion, blistering, or necrosis
Wound Care and Local Treatment

Proper wound care plays a central role in healing.
Basic Wound Management
- Keep the area clean and dry
- Cover with a sterile, non-stick dressing
- Change dressings regularly
Preventing Infection
- Antibiotics are not used preventively
- They are only prescribed if signs of bacterial infection appear, such as pus, spreading redness, or warmth
Avoid Early Surgery
- Surgical cutting or debridement is usually avoided in the early stages
- Early intervention can enlarge the wound and delay healing
Early Recognition of Necrosis
Some bites progress despite appropriate care.
Early warning signs include:
- Darkening skin at the center of the bite
- Increasing pain after several days
- Formation of an open sore
At this stage, treatment remains conservative, with close follow-up and specialized wound care if needed.
Management of Necrotic Lesions

When tissue necrosis develops, treatment emphasizes patience and careful wound handling rather than aggressive intervention. Necrosis often evolves over days, and early surgical removal of tissue can worsen the injury.
Key principles of necrotic wound care include:
- Ongoing gentle cleansing and sterile dressings
- Allowing damaged tissue to clearly demarcate before any removal
- Close follow-up with a healthcare provider or wound care specialist
- Pain control and monitoring for infection
In many cases, the body naturally sheds dead tissue over time. Only after the wound stabilizes is debridement considered, and even then, it is performed conservatively.
Treatment of Systemic Symptoms
Systemic symptoms are uncommon but require prompt medical attention when they occur. Treatment is usually provided in a hospital setting and is tailored to the patient’s symptoms and overall health.
Care may include:
- Intravenous fluids for hydration
- Medications to control fever, nausea, or pain
- Blood tests to monitor red blood cell breakdown and kidney function
- Observation for worsening systemic reactions
Children and older adults are monitored especially closely, as systemic effects can progress more rapidly in these groups.
Antibiotics: When They Are Used
Antibiotics do not treat spider venom and are not routinely prescribed for brown recluse bites. Their use is limited to situations where a secondary bacterial infection is clearly present.
Signs that may justify antibiotics include:
- Increasing redness spreading away from the wound
- Pus or cloudy drainage
- Worsening warmth and swelling
- Fever linked to local infection rather than venom effects
Using antibiotics unnecessarily can delay proper care and contribute to resistance, which is why clinicians are cautious.
Surgical and Advanced Interventions
Surgery is reserved for a small percentage of cases involving severe tissue loss. When needed, it is performed weeks after the bite, not during the acute phase.
Advanced treatment options may include:
- Delayed surgical debridement
- Skin grafting for large or non-healing ulcers
- Reconstructive procedures in rare, severe cases
Outcomes are generally better when surgery is delayed until the wound is stable and inflammation has subsided.
Home Care and Recovery
Recovery from a brown recluse bite often requires time and consistency rather than intensive treatment. Patients are typically instructed on proper home wound care and symptom monitoring.
Important aspects of recovery include:
- Keeping the wound clean and protected
- Avoiding friction or pressure on the area
- Managing pain with prescribed or recommended medications
- Attending follow-up appointments as advised
Healing may take several weeks, and larger wounds can take months. Scarring is possible, particularly after necrotic injury, but often fades over time.
What Treatments Should Be Avoided
Certain interventions have been shown to be ineffective or harmful and should be avoided unless specifically directed by a healthcare professional.
These include:
- Cutting or suctioning the bite
- Applying heat
- Early aggressive surgery
- Unproven antidotes or home chemicals
- Self-directed steroid use
Avoiding these measures is just as important as following recommended care.
Prognosis and Long-Term Outcomes
The overall prognosis for brown recluse spider bites is good. Most bites heal without serious complications, especially when treated appropriately and monitored closely. Severe outcomes are rare, and permanent disability is uncommon.
Factors influencing recovery include:
- Bite location and size
- Speed of treatment initiation
- Age and general health of the patient
- Presence of secondary infection
Even in cases with tissue damage, proper wound care and follow-up usually result in acceptable cosmetic and functional outcomes.